For far too long, obesity has been treated as a simple matter of willpower—a narrative that suggests people just need to “eat less and move more.” But science, experience, and compassionate care tell a very different story.
At Valley Obesity Medicine & Diabetes (VOMD), we understand that obesity isn’t a failure of discipline—it’s a complex, chronic condition influenced by biology, hormones, metabolism, and environment. By taking a metabolic approach to weight management, we can finally shift the conversation from blame to healing—and help people make progress that lasts.
Understanding Obesity as a Disease
Obesity is now recognized by leading medical organizations, including the American Medical Association, as a chronic, relapsing disease. That means it’s not simply the result of choices—it’s the result of multiple factors working together: genetics, hormones, metabolism, stress, sleep, and even medications.
When weight regulation systems in the body stop functioning as they should, the signals that tell us when we’re hungry or full become disrupted. Hormones like insulin, leptin, and ghrelin—key messengers that help manage appetite and energy use—can become imbalanced. The result? Your body may hold on to weight, even when you’re doing “everything right.”
That’s why a purely willpower-based approach doesn’t work. The body has powerful biological mechanisms designed to defend its current weight. Dieting alone can slow metabolism and increase hunger hormones, making weight loss even harder to sustain.
The Metabolic Connection
Metabolism isn’t just how quickly we burn calories—it’s the entire network of processes that convert food into energy. When that system is out of balance, it affects nearly every aspect of health, including blood sugar, inflammation, and cardiovascular risk.
At VOMD, we look at the whole picture of your metabolic health, not just the number on the scale. This includes:
- Body composition analysis to understand fat and muscle distribution
- Review of past medical history and symptoms to see if you have developed complications from obesity
- Examination of current medications to rule out the possibility that some of your medications might have made it difficult to lose weight
- Lifestyle and behavioral assessments of food intake/dietary habits, physical activity, sleep, stress and social determinants of health to narrow down the primary contributing factors for your disease of obesity
- Bloodwork and metabolic testing to screen and assess potential complications of obesity, such as diabetes, liver fibrosis, congestive heart failure, and chronic kidney disease
By identifying the root causes, we can create a treatment plan that supports your metabolism—not fights against it.
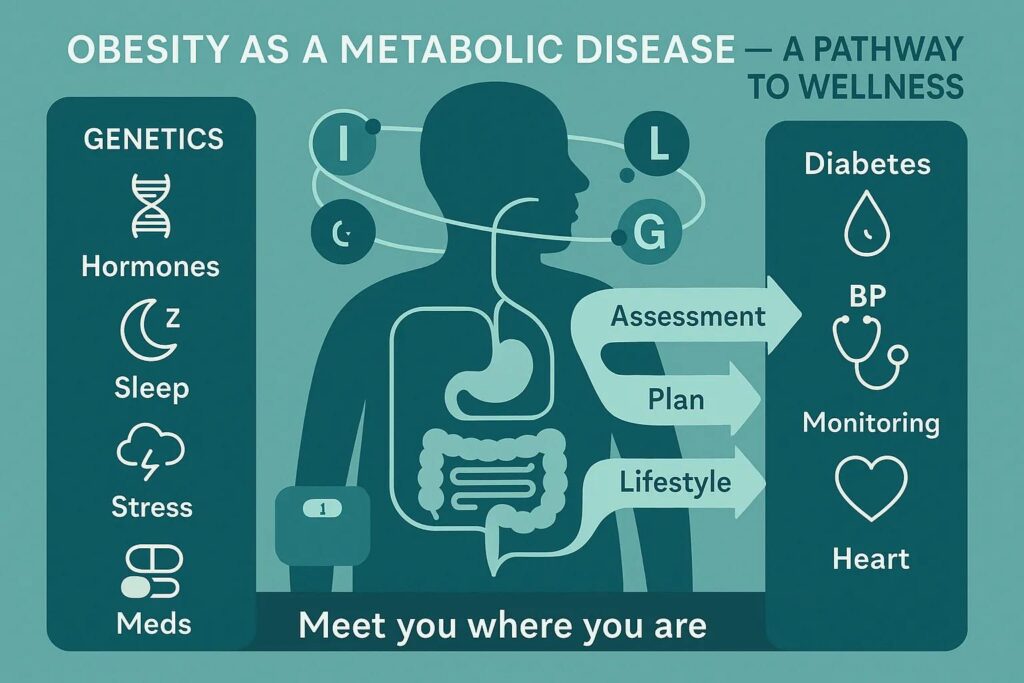
Beyond “Eat Less, Move More”
Lifestyle choices still play an important role in health—but they’re only one piece of the puzzle. Our approach integrates evidence-based medical treatments with personalized coaching and guidance.
That may include:
- FDA-approved medications that help regulate appetite, insulin sensitivity, and metabolism
- Nutrition and movement plans that are realistic, sustainable, and supportive
- Behavioral support to address habits, mindset, and emotional triggers
- Ongoing monitoring to track progress and make adjustments as your body responds
This multi-layered strategy helps patients experience real change—without the guilt or burnout that often comes from short-term dieting.
Why Compassion Matters
Weight stigma is one of the biggest barriers to effective obesity care. When people are made to feel ashamed of their weight, they’re less likely to seek medical help, even though obesity is treatable.
At VOMD, we believe in meeting you where you are. Every journey looks different, and progress is about more than the scale. Our goal is to create a space where patients feel understood, respected, and supported—because compassion is a key part of healing.
As Dr. Michael Li explains, “We don’t just treat numbers on a chart. We treat people.” That means listening to your story, understanding your challenges, and celebrating your progress—every step of the way.
The Link Between Obesity and Other Conditions
Obesity often doesn’t exist in isolation—it’s closely connected to other chronic conditions such as diabetes, high blood pressure, and heart disease. In fact, managing one condition often helps improve the others.
When we approach obesity as a metabolic disease, we also improve insulin sensitivity, lower inflammation, and reduce the risk of long-term complications. Many patients find that as they lose weight and balance their metabolism, they feel more energetic, sleep better, and regain confidence in their bodies.
The goal isn’t just weight loss—it’s whole-person wellness.
Hope in Modern Medicine
The good news is that we have more tools and knowledge than ever before. Today’s generation of obesity medications and metabolic treatments are safer, more effective, and better tailored to individual needs. When combined with lifestyle changes and ongoing support, they can make meaningful, lasting improvements in health and quality of life.
It’s not about perfection—it’s about progress. And progress looks different for everyone. For one person, it might mean lowering blood sugar. For another, it might mean walking without pain or having more energy to play with their kids. Each of those victories matters.
A New Way Forward
Reframing obesity as a metabolic condition opens the door to better outcomes and greater self-compassion. When we stop blaming willpower and start understanding biology, we can begin to treat the true root causes—and help people achieve sustainable, lifelong health.
At Valley Obesity Medicine & Diabetes, we combine medical expertise, empathy, and evidence-based care to empower patients on their wellness journeys. Because lasting change starts when you have the right support, the right tools, and the right understanding of your body.
If you’re ready to take that first step, we’re here to walk with you.
